Covid-19 and Chronic Fatigue Syndrome

COVID-19 and Chronic Fatigue Syndrome
The covid-19 pandemic has affected a significant portion of people. Even after recovery from coronavirus infection some people can barely feel energized. Doctors classify this Post-COVID-19 Fatigue Syndrome.
The characteristics of post-COVID19 fatigue syndrome are similar to Myalgic Encephalomyelitis or Chronic Fatigue Syndrome (ME/CFS). Different health conditions correlated with coronavirus infection also sap your energy, leaving you feeling sluggish and listless similar to chronic fatigue syndrome (CFS), also called myalgic encephalomyelitis.
Chronic fatigue after acute respiratory illness has scaled up at a high rate due to long Covid-19 infection. Post-viral fatigue occurs commonly after any type of viral infection such as a bout of flu or battling off an Epstein-Barr virus. Many people experience persistent fatigue for a few weeks, or even months, after recovery from viral infection. This prolonged fatigue is unpleasant and doctors focus on an eventual return to full health.
Unfortunately for some patients, the fatigue does not cure completely. Viral infections are considered one of the primary causes of myalgic encephalomyelitis (ME) or chronic fatigue syndrome (CFS). This chronic condition is described as extreme tiredness, along with brain fog, sore joints, and flu-like symptoms.
Covid-19 has spread worldwide and around one in ten recovered patients are experiencing post-viral symptoms such as CFS at least three months later.

What is Chronic Fatigue Syndrome?
Chronic fatigue syndrome (CFS) is a long-term or chronic condition. This is characterized by fatigue that worsens with exertion making you feel very tired. This interrupts your normal, daily activities, and does not improve with rest.
Younger and middle-aged women are more prone to CFS, but people of any age or gender could develop it. Genetics might also play a key role.
Numerous viruses are linked to ME or CFS leading to establish persistent and chronic infections. The viral infection causes chronic low-level inflammation that would activate cell-mediated immunity. This leads to an increase in inflammatory mediators that contribute to the symptoms including fatigue, fever, sleep, and cognitive disorders. Irregularity of immune has been observed that involves a change in cytokine profiles along with immunoglobulin levels (T- and B-cell) and a decrease in natural killer cell cytotoxicity.
People between the age of 40s and 50s are prone to develop CFS after a covid-19 illness. Women are more likely (almost 2-4 times) to develop CFS than men. Some of the other factors that increase your risk for CFS include:
Genetic predisposition
Allergies
Stress
Environmental factors
What causes Chronic Fatigue Syndrome?
The mechanism triggering chronic fatigue syndrome is unknown. Covid-19 infection persisting for a long time supposedly triggers chronic fatigue symptoms. It can trigger potentially by:
Viral infections: It is likely that some viruses like coronavirus trigger CFS in some people. Suspicious viruses include the Epstein-Barr virus, human herpesvirus. No conclusive link has yet been found.
Immune system problems: People suffering from Covid-19 have impaired immune system that makes them prone to develop chronic fatigue syndrome. But, it's unclear if this impairment alone is enough to cause the disorder.
Hormonal imbalances: People who have chronic fatigue syndrome also experience abnormal blood levels of hormones produced in the hypothalamus, pituitary glands, or adrenal glands.
Physical or emotional trauma: Sometimes, you might have an injury, surgery, or significant emotional stress shortly before the symptoms began.

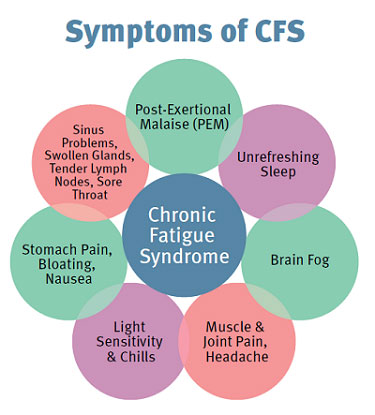
What are the symptoms of Chronic Fatigue Syndrome?
Characteristic symptoms of CFS may vary from person to person. The severity of symptoms fluctuates every day. Symptoms of CFS include:
Fatigue
Problems with memory, focus, or concentration
Sore throat
Headaches
Enlarged lymph nodes in your neck or armpits
Unexplained muscle or joint pain
Dizziness worsening with moving, lying down, sitting, or standing
Unrefreshing sleep
Extreme exhaustion after physical or mental exercise
Tender and swollen lymph nodes in your neck and armpits
How to Diagnose Chronic Fatigue Syndrome?
To diagnose CFS doctor would rule out the potential causes and analysis your medical history. The doctor would confirm the core symptoms to confirm CFS such as the duration and severity of your unexplained fatigue.
The key part of diagnosis is to rule out other potential causes such as Mononucleosis, Lyme disease, Multiple sclerosis, Lupus (SLE), Hypothyroidism, Fibromyalgia, depressive disorder, obesity, and Sleep disorders.

How can CFS be treated?
Currently, the doctors are not able to find a cure or approved treatment for myalgic encephalomyelitis or chronic fatigue syndrome (ME/CFS). Doctors focus on treating or managing the symptoms. Treating or managing these symptoms would provide relief for some but not others. For others learning new ways to manage activity can be helpful.
Healthcare providers target the symptom that causes the most problems. The device the treatment plan to provide possible benefits through medicines and other therapies. Healthcare providers would not be able to able to work on the symptoms alone but need to support your family. Healthcare providers and families understand that the treatment process might be hard on people suffering from ME or CFS. The treatment plan would include:
Home remedies and lifestyle changes: Limiting or eliminating the caffeine, nicotine, and alcohol intake would induce sleep better and ease your insomnia. It is important to avoid napping during the day if it’s hurting your ability to sleep at night and create a sleep routine. You should go to bed at the same time every night and wake up around the same time every day.
Medications: No specific medication can provide relief from associated symptoms. The symptoms may change over time, so your medications may have to as well. CFS can trigger depression thus doctors may prescribe low-dose antidepressant therapy or a referral to a mental health provider. fromThe doctor would prescribe sleep aid medicines if lifestyle changes don’t give you a restful night’s sleep. Pain-reducing medication provides relief from aches and joint pain caused by CFS.
Cognitive Therapy: This aims at improving mental health with the help of psycho-social interventions. Cognitive therapy focuses on changing cognitive distortions and behaviors, improving emotional regulation, and developing personal coping strategies that help in providing relief from covid-19 related issues.
Orthostatic intolerance: Some of the symptoms of chronic fatigue syndrome such as feeling faint or nauseated when you stand or sit upright are common among adolescents. Medications to regulate blood pressure or heart rhythms may provide relief from such symptoms.

Managing post-exertional Malaise (PEM)
Covid-19 patients often experience PEM, which is the worsening of symptoms after even minor physical, mental or emotional exertion. In severe cases, sensory overload such as light and sound can also induce PEM. The symptoms might worsen 12 to 48 hours after the activity or exposure and can last for days or even weeks.
Doctors address PEM cases by activity management or pacing. Pacing aims to balance rest and activity to avoid PEM flare-ups often caused by exertion that Covid-19 patients cannot tolerate. This requires you to find your limits for mental and physical activity and staying within the “energy envelope”.
Outlook
Covid-19 can lead to various health conditions that cause long-lasting fatigue, including chronic fatigue syndrome. Talk to your health care provider if you’ve been feeling tired for more than six months. They can get to the root of the problem and get your energy back.
If you or anyone you know is suffering from the after-effects of Covid, our expert providers at Post Covid Centers will take care of your health and help you recover.
Call us on (469) 545-9983 to book a telehealth appointment for a home check-up.
Post Covid Syndrome vs. Fatigue
While COVID-19 is a short-lived disease in most people, others experien...
Post Covid Syndrome vs. Skin Weakness Problems
A new study illustrates that some patients with COVID-19 disease have continuous skin-associated symptoms...
RELATED BLOGS
