What is Asymptomatic and Mild COVID-19?
As the coronavirus pandemic continues, we are learning more about how various groups are experiencing COVID-19. Everyone is speaking about mild, moderate, and severe cases and critical cases. What does this mean?
There are, as yet, no clear guides for patients to tell them what doctors or primary care physicians mean by mild, moderate, or severe COVID-19. Some guidance on classifying disease is appearing in research papers and epidemiological reports, but it is not very specific. For instance, the broad definition of moderate disease seems to be that it is worse than the mild disease but not severe.
How have people “categorized” COVID-19?
You will have heard in public health announcements and in the media that some people have had mild COVID-19 infections, and others moderate, severe, or serious.
Yet, when you look up the symptoms, you are told to expect a cough, a temperature, and a loss of (or change to) your sense of smell and/or taste. How bad cough is a mild case? How much of a temperature is severe?
The terms usually used to classify the disease are:
Mild
Moderate
Severe
Critical
These classifications are constant with published descriptions so far. If formal, agreed with the guidance on what we call mild, moderate, and severe cases are published or presented, these might differ slightly. For now, this looks to be fit the way the terms are being used.
Each of these 'levels or grades' of disease is much less common than the preceding one (so severe is less common than moderate, which is less common than mild, and so on).
Who gets what?
Most young and healthy persons are likely to belong to the asymptomatic or mild group 1 or 2. Although, some young healthy people have become very unwell and some have died. In percentage terms, this seems to be very low, but the chance is not zero.
You have a bigger chance of moving further down the list into moderate, severe, and critical infections if:
You are over 60 years (and higher still if you are over 70 years) the risks increase with increasing age, regardless of how healthy you are; or
You have another medical condition which means you have been instructed to shield.
To a lesser extent, if you have a medical condition that makes you clinically susceptible; or
You are of BAME origin (some of the increased likelihood of people of BAME origin being seriously affected appears to associate with their likelihood of having hidden medical conditions, working in public-facing jobs, living in more crowded or populous conditions, etc).
Remember, each of the 'levels or grades' of disease is much less common than the preceding one.
Even in the over-80s group, very significantly more individuals will have mild or moderate diseases than the severe disease.
Not an exact science
You might well not fit anyone’s classification exactly. You might be between two. You might move from mild to moderate symptoms, then back to mild symptoms. You could experience symptoms in more than one group. The disease is like that.
When huge numbers of individuals are affected, they will not all fit perfectly into simple group classifications of mild, moderate, or severe. But if your symptoms are predominantly of mild illness with, say, one or two moderate features, you might be 'mild to moderate.
If your symptoms are primarily moderate, but you are clearly getting worse and begin to get symptoms that look to fit 'severe', do not wait to look for urgent help till you have more of the severe symptoms.
In each category, most individuals will not progress to the next. You are more likely to progress if you are susceptible, especially if you are over 60 years. If you are in a very susceptible or vulnerable group and you think you have even mild COVID-19, you should seek advice.
How bad is my COVID-19?
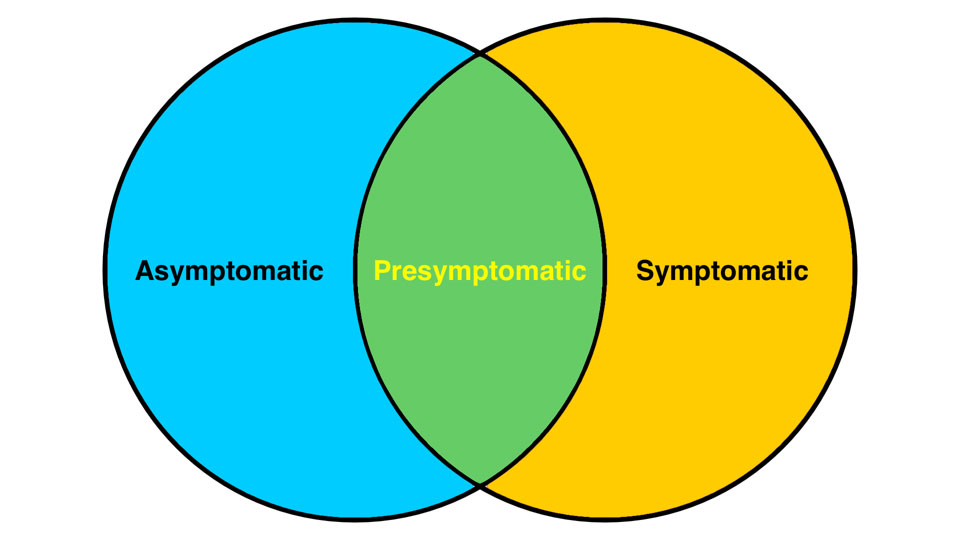
Asymptomatic COVID-19
The government guidelines recommend that one in three people who have COVID-19 have no symptoms. It seems that this happens more usually in the healthiest and the younger age groups, including most children.
Antibody testing helps us to understand how many people have had coronavirus unknowingly or incidentally, with or without symptoms. At the moment, whether you could book antibody testing depends on your job and where you live. In most situations, it is not available on the National Health Service (NHS).
Being asymptomatic signifies that you have no symptoms. If you live in a house with people with a COVID-19 infection and you have no symptoms, you might be an asymptomatic case. Although, recent research indicates that the proportion of people who remain completely asymptomatic is lower than first thought, at about one in five people.
And while people with the asymptomatic infection are less likely than those with symptoms to spread the illness, the risk is by no means non-existent. This is why self-isolating for the whole ten-day period from your last contact with someone with a known infection is so crucial.
Remember, this entire pandemic possibly started with one case. Do not be a spreader.
Mild COVID-19
The virus affects primarily your upper respiratory tract, mainly the large airways. Key symptoms are temperature, a new, persistent cough, and/or a loss of your sense of smell or taste.
Patients with mild disease have flu-like symptoms. These might include a dry cough and mild fever, but the fever might not reach 37.8°C, and there might sometimes be little or even no cough. Patients may notice a feeling of being a bit more breathless than normal on exercise, but they are not out of breath on common household activity.
With mild COVID-19:
You might have a fever, including one that does not reach the 37.8°C mark or degrees.
You run the risk of losing your smell and taste.
You might have tiredness, muscle aches, or a headache.
You are not highly likely to have a sore throat or runny nose, but they do happen in some cases.
You do not have marked breathlessness.
Your self-care, cooking, eating, and drinking is not affected. Your appetite is normal or pretty normal.
You might feel sad or weepy.
The symptoms generally seem to last about seven to ten days.
Most normally healthy people under 60 years who have symptoms will have this form.
Most (81 percent) of symptomatic COVID-19 cases are mild and remain mild in severity. Although, patients with the mild disease could deteriorate, sometimes quickly, and this is more likely in at-risk groups.
When to seek help
If you think you might have COVID-19 or that you have been exposed to the coronavirus, you should stay at home and self-isolate. At the moment, only people with symptoms or in specific other limited circumstances are eligible for a COVID-19 test, but if these apply to you, book a test.
The vast majority of individuals with mild or asymptomatic infections do not require to seek for medical attention and could treat their symptoms at home. There are some situations in which you must speak with a clinician about your symptoms. Although, do not simply show up at your general practitioner (GP) surgery or a pharmacy as you risk spreading the virus to others. Instead, call first and seek advice.
If you are in a vulnerable or susceptible group, look for advice. This includes all individuals who are being 'shielded' for their own protection.
If you experience symptoms of COVID-19, consult a doctor over the phone and you:
Are over 70 years (not all over-70s are in the shielding category, but you are at increased risk of severe disease).
Have a major heart, lung, or kidney disease, or immune deficiency.
Are on oral steroids.
Have had a solid organ transplant.
Are invited every year for a National Health Service (NHS) flu vaccination because of your own medical condition (this does not apply if you are provided a flu vaccination because you are a carrier and does not apply to children).
COVID-19 could worsen quickly. Vulnerable or susceptible people should not manage their COVID-19 alone by depending on written advice. Written advice can’t check up on you. Government advice is continuously updated. Additional advice for shielding and extremely vulnerable or susceptible people are also found here.
If you have symptoms that are worsening, look for advice. This is especially true if you have any of the severe features. People with COVID-19, especially those in risk groups, could deteriorate from mild to moderate to severe. Similarly, if you are afraid, please look for advice. That is why our health professionals are there for.
You might have to call National Health Service (NHS) 111 (or the relevant number in your region) and wait to speak with a nurse. You could also use National Health Service (NHS) 111's online tool to find out what to do next if you think you have COVID-19. In case of an emergency, call 999 and ask for an ambulance. Inform the call handler that you think that you have coronavirus.
If you or anyone you know is suffering from asymptomatic covid, our expert providers at Post Covid Centers will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for a home check-up.
Post Covid Syndrome vs. Fatigue
While COVID-19 is a short-lived disease in most people, others experien...
Post Covid Syndrome vs. Skin Weakness Problems
A new study illustrates that some patients with COVID-19 disease have continuous skin-associated symptoms...
RELATED BLOGS
